Improve Strength, Stability, Mobility & Balance
At Perth Sports Physio we have been treating knee injuries at elite level for 20 plus years. We have seen all forms of injury from arthritis to Iliotibial Band (ITB) Syndrome. We know how to reduce your knee pain and then build your strength and flexibility back up to allow you to return to your goals in sport or home activities.
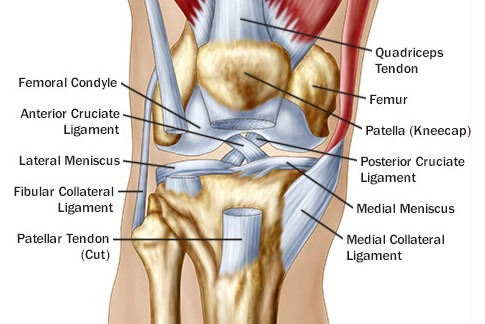
The knee is a complex arrangement of firstly bones, cartilages, ligaments surrounded by tendons and supported by a sleeve of synovial membrane that secretes lubricating fluid into the joint. It is a living structure requiring nutrition through the supplying blood vessels. Any of these structures can be affected by injury or other abnormality giving rise to symptoms.
Examination
First we discuss with you what you have done and what you feel are your problems. Then we thoroughly examine the knee with a range of tests of anatomical structures. We may arrange scans for your knee if we think there is an internal problem that needs further investigation to clarify the degree of injury.
First Treatment
After the knee has been diagnosed the aim is to reduce pain in your knee in the first treatment session. This may involve patella taping, bracing, massage, icing, dry needling and strapping.
Rehabilitation Plan after new injury or After Surgery
The next phase of treatment involves planning the course of rehab to return you to full fitness goals. Whether it be getting back to a walk with the dog or playing with the grandkids or running on the wing in rugby.
We may give you a 6 phase programme from the initial insult to return to play. The programthat involves:
- strength
- balance
- flexibility
- cardiovascular fitness options
- control of the biomechanics at your foot and hip that can effect your knee pain
- improving power and speed and agility
- return to your sport skill or goal
The following is a widely quoted list of the likely cause of pain at various sites around the knee:
Anterior knee pain (at the front):
- Patellar tendonitis (jumper knee)
- Quaricep tendon injury
- Patellar maltracking
- Chondromalacia patella
- Patello-femoral osteoarthritis
- Patellar maltracking or instability
- Osgood Schlatter’s syndrome
- Runners knee
Medial knee pain (on the inner side):
- Torn or degenerate medial meniscus
- Medial plica
- Medial ligament injury
- Cartilage damage on the medial femoral condyle
- Medial compartment osteoarthritis
- Pes anserinus bursitis
Lateral knee pain (on the outer side):
- Torn or degenerate lateral meniscus
- Lateral ligament injury
- Postero-lateral corner injury
- Damage to the lateral facet of the patella
- Lateral compartment osteoarthritis
- Iliotibial Band (ITB) Syndrome
Posterior knee pain (at the back):
- Posterior horn meniscal tear
- Baker’s cyst
- Hamstring injury
- Osteoarthritic change
- Calf strain
The whole Knee:
- Oseoarthritis
- ACL Rupture
- Tibial Fracture
- Femoral fracture
In diagnosing knee pain it is also important to identify its character as this also provides clues as to its cause. The following is a widely quoted list of the different types of pain at various sites around the knee:
- Constant pain around the whole knee
- Sudden sharp pain usually well localised
- A burning sensation
Constant pain involving the whole knee is usually due to an inflammatory arthritis such as rheumatoid or gout and can sometime occur in tri-compartmental osteoarthritis. Osteoarthritic pain often occurs at rest and at night. It can improve initially on exercise becoming more severe after longer periods walking or on more strenuous exercise.
Sudden sharp pain is usually well localised and generally implies a mechanical problem such as a torn meniscus or a loose body.
Burning pain is usually inflammatory in origin and can also be seen in neurological abnormalities such as neuropathies affecting the leg. In neuropathies the pain tends to be in a stocking distribution and described as burning, stabbing, prickling, or tingling.
Swelling
Chronic swelling is usually due to an inflammatory arthropathy or osteoarthritis but can occur following untreated internal derangements of the knee following trauma.
Rapid swelling that happens within minutes or a couple of hours after injury almost always means bleeding has occurred into the knee. A slower onset over 24 hours is usually due to the secretion of excess synovial fluid following trauma.
The commonest cause of bleeding into the knee is an anterior cruciate ligament injury, but rapid swelling can also occur following meniscal tears and intra-articular fractures.
Common inflammatory conditions that affect the knee and give rise to chronic swelling include:
- Rheumatoid arthritis
- Gout
- Septic arthritis
(infection)
Giving way
What we mean is that the knee suddenly bends causing you to have to hold on or indeed fall over sometime. If you actually fall we would tend to call that complete collapse of the knee
Episodes of giving way, associated with pain and clicking often indicate a piece of torn meniscus becoming trapped within the joint or sometimes a loose body made of bone or cartilage.
Giving way can also be due to a ligament injury especially the anterior cruciate and less commonly the medial ligament or posterior cruciate.
Locking
What we mean is that the knee will not move beyond a certain point. Locking can be quite a painful experience. Most commonly the knee will bend reasonably well but will not extend fully. This is usually due to something jamming in the joint. Sometimes a locked knee can be self manipulated or gently persuaded into moving again. Sometimes a locked knee settles quite spontaneously even on occasions on sleeping when the muscles relax.
Locking is a mechanical problem and points to a diagnosis of meniscal tear or loose body but can also occur in the presence of a plica or thickened fold of material within the knee. A loose piece of cartilage within the knee can also cause it.
Locking should be distinguished from chronic reduction in range of movement secondary to osteoarthritic problems and from stiffness due to the presence of a large amount of fluid within the joint.
Stiffness
What we mean is that the knee can be moved but with difficulty. Slow painful movements often associated with generalised knee pain are a characteristic of inflammatory problems or osteoarthritis. Stiffness is frequently encountered first thing in the morning on getting out of bed and can also be a feature after sitting in the same position for some time.
